The field of pathology is experiencing a rapid transformation, driven by innovations like molecular diagnostics, genomics, and digital pathology. While these advancements promise greater precision and efficiency in patient care, they also introduce a complex set of regulatory and quality challenges that modern pathology labs must navigate. Staying compliant and maintaining a high standard of quality is crucial for accurate diagnosis and patient safety.
🚧 The Regulatory Hurdle: A Moving Target
The regulatory environment for pathology is anything but static. Laboratories must comply with a myriad of standards, often from multiple bodies, which can be challenging to harmonize.
- Evolving Oversight: Regulations are constantly updated to keep pace with new technologies. For instance, the discussion around the oversight of Laboratory Developed Tests (LDTs)—assays designed, manufactured, and used within a single laboratory—highlights a significant area of regulatory uncertainty and potential burden. Increased regulation, while aiming for quality, risks stifling innovation or limiting patient access to crucial, specialized testing, especially for rare diseases.
- Harmonization and Standardization: Pathology services often face challenges due to a lack of harmonization and standardization, leading to variations in service provision and reporting across different labs. The need for international standards, like those outlined in ISO 15189 (requirements for quality and competence in medical laboratories), provides a framework but requires significant internal effort to implement consistently.
- Data Privacy and Security: The digitization of patient information necessitates strict adherence to data privacy regulations (like HIPAA in the US) to protect sensitive patient data. Labs must invest in robust cybersecurity measures to prevent breaches and ensure data integrity across interconnected systems.
📈 Quality Assurance in the Age of Digital Pathology
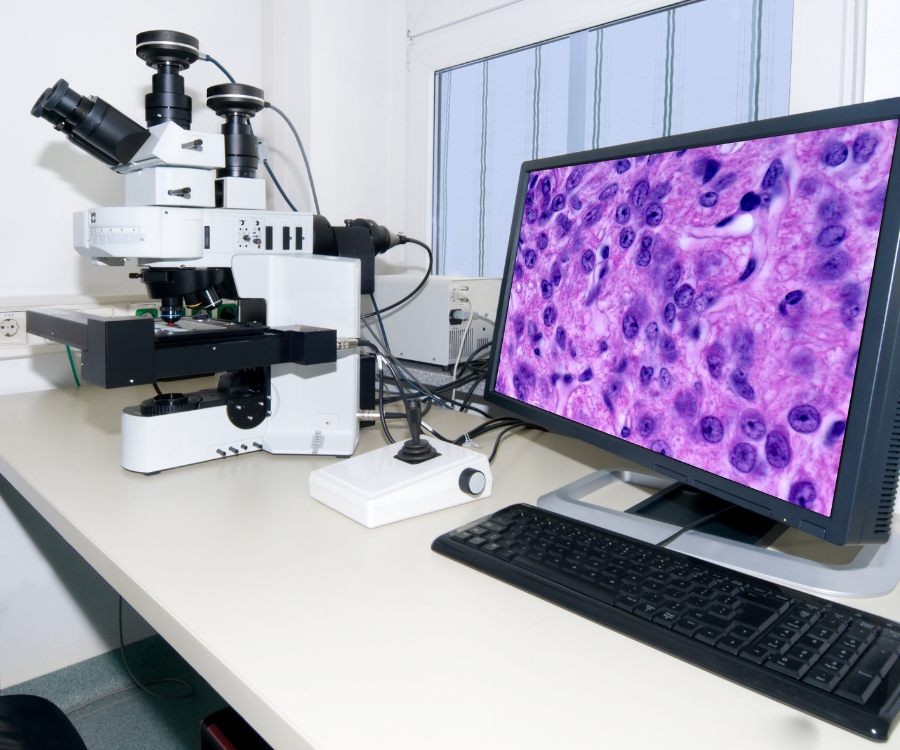
The shift to digital pathology (DP), where glass slides are scanned into high-resolution images, brings its own set of unique quality management challenges.
- Image Quality and Validation: Ensuring that the quality of whole-slide images is consistent and diagnostically equivalent to traditional microscopy is a primary concern. Labs need to establish clear quality control (QC) procedures for scanners, monitors, and image processing to ensure accurate results.
- Massive Data Management: Digital pathology generates enormous files (Whole-Slide Images or WSIs), creating a massive burden on IT infrastructure, storage, and data backup systems. Developing scalable and cost-effective data management strategies is essential for sustainable DP adoption.
- AI Integration and Validation: The introduction of Artificial Intelligence (AI) algorithms for image analysis and diagnostic assistance adds another layer of complexity. Labs must validate the performance of these AI tools, address potential algorithmic bias, and establish clear protocols for human oversight to ensure that the final diagnosis remains the pathologist’s responsibility.
✅ Building a Robust Quality Management System
To successfully meet these modern challenges, pathology labs need a forward-thinking and robust Quality Management System (QMS) that goes beyond minimum compliance.
- Continuous Training and Workforce Development: With new molecular and digital technologies, there is an urgent need for continuous training to equip the existing pathology workforce with the necessary technical skills and expertise to manage complex equipment and data.
- Integration and Interoperability: Modern pathology relies on seamless communication between instruments, Laboratory Information Systems (LIS), and Electronic Health Records (EHRs). Quality is improved when systems are fully integrated, minimizing manual data transfer and the risk of error.
- Culture of Quality and Transparency: Ultimately, quality starts with a commitment from leadership. A QMS should foster a culture of continuous improvement, where errors are viewed as learning opportunities and the focus shifts from meeting minimum standards to achieving aspirational excellence in patient care.
The path forward requires investment in technology, training, and a collaborative approach with regulators and industry partners to ensure that innovation is balanced with unwavering quality and patient safety.